Blood Clots during Pregnancy: What you should know
Posted by KELSEA FRANZKE

Blood clots can be a serious health concern for anyone, and those concerns are elevated for those who are pregnant. Complications surrounding blood clots can affect both your health and your baby’s health if they occur while pregnant, and when left untreated, blood clots can be life threatening for you and your baby.
Fortunately there are steps and preventative treatment options you can take to minimize your risk of developing and experiencing a blood clot during pregnancy.
What is a Blood Clot?
When your body sends platelets to block the flow of blood, a blood clot occurs. Typically this will occur if you have a cut or wound, and your body is working to stop the injury from bleeding.
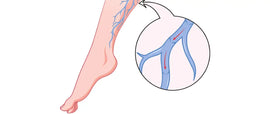
A blood clot that occurs in the deep vein, also known as a Deep Vein Thrombosis (DVT), is a condition that often occurs in the lower legs, thigh, arm or pelvis.
It is important to recognize when a DVT occurs because when left untreated, it can break off and travel to the lungs which may cause a blockage called a Pulmonary Embolism. This can prevent the blood from reaching the lungs and can result in death. A Deep Vein Thrombosis and Pulmonary Embolism are experienced by 2-5% of people in their lifetime.
Symptoms of Deep Vein Thrombosis
DVT can cause leg pain, but it often occurs without any symptoms. Nearly 50% of all DVT cases do not have recognized symptoms, but the following are some to be aware of:
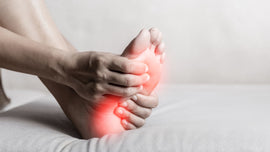
- Swelling in the affected leg - this includes swelling in your ankle and foot
- Pain in your leg - this can include pain in your ankle and foot
- Pain starting in your calf which feels like cramping or a charley horse
- Warmth over the affected area
- Changes in your skin colour such as turning pale, red or blue
Symptoms of a blood clot in your lung may include:
- Difficulty breathing
- An irregular heartbeat, or a heartbeat that is faster than normal
- Chest pain that gets worse when you cough or take a deep breath
- Coughing up blood
Blood clots and pregnancy: Why is there a higher risk?
Changes in your body that occur naturally during pregnancy, childbirth and 3-months after delivery can put you at a higher risk for a blood clot due to the impacts of pregnancy on your blood circulation.
During pregnancy, your blood clots more easily to lessen blood loss during labor and delivery. People may also experience less blood flow to their legs later in pregnancy because the blood vessels around the pelvis are pressed upon by the growing baby. Additionally, decreased movement due to bed rest after delivery can limit blood flow in the arms and legs, increasing a risk for a blood clot.
In fact, people who are pregnant have a 6-times higher risk of developing blood clots (DVT) than those who are not pregnant. Factors unique to pregnancy that can contribute to the development of blood clots include:
- When pregnant, your blood volume increases by 30-50% which puts a strain on the circulatory system.
- An increase in the hormone progesterone relaxes the lining of the veins and slows venous return.
- As the baby grows, it puts pressure on the inferior vena cava, a large vein that collects blood from the lower body. This increases the blood pressure in the lower body putting pressure on the vein walls.
- Slower blood flow increases the risk of developing DVT.
On average, 1-2 people in 1000 will develop DVT or pulmonary embolism during pregnancy.
Know your risk
Pregnancy is one factor that can put people at a higher risk for developing a blood clot, but there are also other factors that come into play:
- Personal history or family history of blood clots or a blood clotting disorder
- Prolonged immobility - having a decrease in physical movement by being on bed rest or general immobility from pregnancy
- Delivery by C-Section
- Various complications during pregnancy and delivery
- Some long-term medical conditions such as diabetes or lung and heart conditions
Your likelihood of developing a blood clot increases with the number of risk factors you may have. Always speak to your doctor about your health and use resources such as this Blood Clot Risk Checklist for Pregnant Women to help determine your risk.
How to prevent and treat blood clots
Prevention of DVT during pregnancy is very important and fortunately, can be achieved by healthy lifestyle habits including:
1) Staying Active
Physical activity can help with blood circulation. Always speak with your doctor first about what exercises are appropriate for you to do while pregnant. If you are immobile for long periods of time, try to move around or exercise your legs frequently.
2) Wearing Compression Socks
Compression socks alleviate and prevent many common symptoms of pregnancy such as swollen feet and ankles, as well as tired and achy legs.
Wearing Compression Socks increases blood circulation and reduces the risk of blood clots both during pregnancy and after delivery. Dr. Segal’s Compression Socks promote leg health during and after pregnancy! The 15-20 mmHg compression socks provide the right level of compression for during pregnancy and after delivery.
3) Drinking plenty of liquids
It is recommended that while pregnant, people drink 10, eight-ounce glasses of liquid every day, and 12-13 glasses of liquid every day if breastfeeding.
4) Talking to your doctor
Work with your doctor to reduce your risk of blood clots, especially if you are on bed rest, have had a C-section, or have a family history of blood clots. If you are at an increased risk for blood clots, your doctor may prescribe an anticoagulation medicine, also known as a blood thinner, which does not affect your developing baby.
Always speak with your doctor before making any decisions about your health.
SOURCES:
TAGS:
SHARE: